Appearing at the Medicines and Healthcare products Regulatory Agency (MHRA) press conference on 7 April, Deputy Chief Medical Officer Professor Jonathan Van-Tam spoke about vaccine safety. He said: “In a scenario of low exposure... you can see that if you look at the 20 to 29 age band, then the potential benefits [of the Oxford/AstraZeneca Covid-19 vaccine] amount to 0.8 ICU admissions averted compared with serious harms of potentially 1.1.”
However the Telegraph, the Sun and the Evening Standard all seem to have misunderstood these comments.
The Telegraph article appears to be referring to these words when it says: “On April 7, Jonathan Van-Tam, the deputy chief medical officer, presented data at a televised press conference, showing that when Covid-19 is low in the community the risk of developing a blood clot for the under-30s increases.”
The Sun repeated this almost verbatim, stating: “On April 7, deputy chief medical officer Jonathan Van-Tam presented data, showing that when Covid is low in the community, the risk of developing a blood clot for the under-30s increases.”
Again, the Evening Standard’s article made a similar claim, stating: “On April 7, Jonathan Van-Tam, the deputy chief medical officer, shared data at a press conference that showed when Covid-19 is low in the community, the risk of developing a blood clot for the under-30s increases.”
But this is not quite right. The extremely low risk of developing a blood clot after vaccination does not change according to how widespread Covid is. What changes is the balance between the risk of getting very ill with Covid and the risk of getting very ill after vaccination.
Put simply, the chance of getting a serious blood clot after receiving the AstraZeneca vaccine is extremely small. In comparison, the chance of catching Covid and getting seriously ill is much greater for most people. This means that it is much safer to get vaccinated, because it takes away most of a larger risk while adding a very small one.
However, young people who catch Covid are much less likely to become seriously ill, and even less likely to become seriously ill with Covid when the disease itself is very scarce, because there’s little chance of catching it in the first place.
Professor Van-Tam was describing a situation like this, where the risk of a young person catching Covid and getting seriously ill becomes so small that it is even smaller than the risks from vaccination. In that situation, for those people, the risks of the AstraZeneca vaccine might outweigh the benefit.
In early April the MHRA issued a statement recommending that those at higher risk of blood clots because of a medical condition should be considered for the AstraZeneca vaccine only if benefits from the protection against Covid-19 infection outweighs these risks. The Joint Committee on Vaccination and Immunisation (JCVI), which advises government health departments on these matters, also recommended that, on balance, it’s “preferable” that adults under 30 (with no underlying health conditions that put them at higher risk of Covid-19) be offered a different Covid-19 vaccine, such as Pfizer or Moderna, if it’s available.
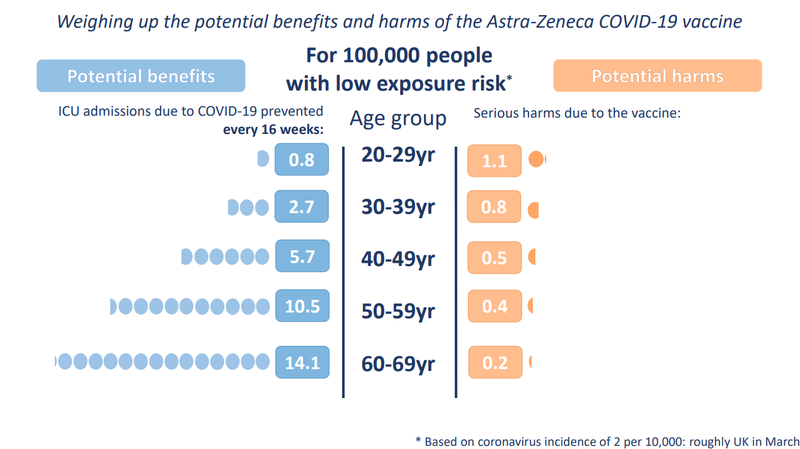
This data visualisation, prepared by the University of Cambridge’s Winton Centre for Risk and Evidence Communication, shows how the balance of these risks will change for different groups, as the prevalence of Covid changes.
This graphic shows the potential benefits and harms of the AstraZeneca Covid-19 vaccine for 100,000 people with low exposure risk (low prevalence of the virus in the community). The potential benefit for 20-29 year olds is 0.8, and the potential harm is 1.1.
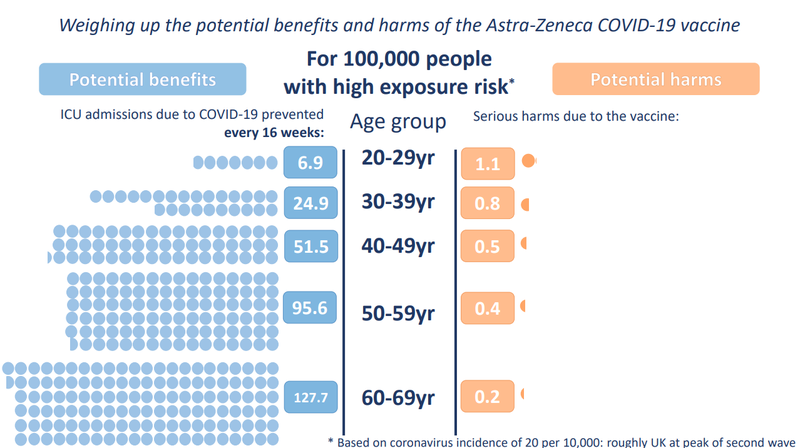
This graphic shows the same information, but for 100,000 people with a high exposure risk (higher prevalence of the virus in the community). As you can see, the potential benefit has risen to 6.9, but the risk has remained static at 1.1.